What Is Endometriosis?
Author: Nnenna Chiloli, MBBS, MPH
Medical Reviewer: Azuka Chinweokwu Ezeike, MBBS, FWACS, FMCOG, MSc (PH)
Highlights
- Endometriosis affects 1 in 10 women of reproductive age worldwide
- Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus
- Common symptoms include painful periods, pelvic pain, pain during sex, bowel symptoms, and infertility
- Diagnosis is based on medical history, physical examination, imaging, and laparoscopy
- Treatment options include pain medications, hormone therapy, surgery, and fertility treatments.
- Although there is no cure, symptoms can be effectively managed with proper care
- Early diagnosis and long-term management improve the quality of care
Introduction
If you‘ve been experiencing painful periods or pelvic pain that disrupts your daily life, you are not alone. Endometriosis is a common condition that affects about one in ten women of reproductive age worldwide. Unfortunately, there’s an average of 6.7 years' delay in the diagnosis, resulting in unnecessary suffering. Understanding what endometriosis is and how it affects your body is an important first step toward getting the right care and finding relief.
Endometriosis happens when tissue similar to the lining of your uterus grows outside the uterus, usually in your pelvis [1,2]. This tissue responds to your monthly hormones just like the lining inside your uterus does, causing inflammation, pain, and sometimes other problems.
The good news is that with proper diagnosis and treatment, many women can manage their symptoms and live a full, active life. This article will help you understand what endometriosis is, recognise its symptoms, and learn about the available diagnostic and treatment options.
How Endometriosis Affects the Body
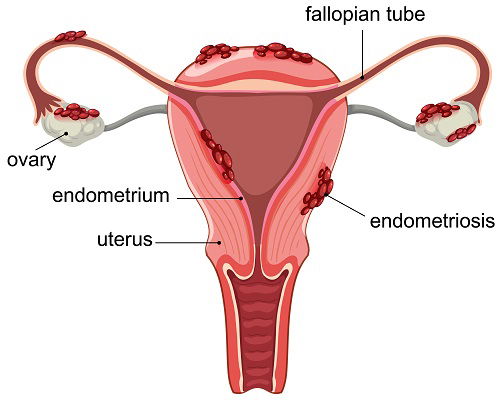
Normally, the lining of your uterus thickens each month to prepare for pregnancy. If pregnancy doesn’t occur, this lining sheds during your period. With endometriosis, tissue similar to this uterine lining grows in places where it shouldn’t be, most commonly on your ovary, fallopian tubes, the outer surface of your uterus, and other pelvic organs [2]. It can also occur outside the pelvis, i.e, the chest, brain, etc.
This misplaced tissue behaves like the lining inside your uterus. It responds to your monthly hormones, thickens, breaks down, and tries to shed.
But unlike the lining of your uterus, this tissue has no way to leave your body, thereby causing the following:
- Inflammation and irritation
Each month, the tissue responds to hormones and irritates the nearby organs, causing swelling and pain
Over time, repeated inflammation can form scar tissue that makes organs stick together, causing more pain and sometimes affecting how they work [3].
- Cysts on the ovaries
Blood can collect in the ovaries, forming cysts called chocolate cysts (endometriomas) because of their dark, thick appearance
- Chronic pain signals
The ongoing inflammation can make nerves in your pelvis more sensitive, leading to chronic pain even when lesions are small
Endometriosis can also affect fertility. The inflammation, scar tissue, and changes in your pelvis can affect the quality of the egg. It can also make it harder for an egg to travel through the fallopian tubes or implant in the uterus.
Common Signs and Symptoms
Endometriosis affects women differently. Some women have severe symptoms, while others have few or no symptoms at all. The amount of endometriosis tissue doesn’t always match the level of pain. Some women with small amounts of tissue have severe pain, while others with more extensive disease have mild symptoms.
Common signs of endometriosis are:
- Pelvic pain
This includes:
- Painful periods that may be enough to keep you from work, school, or daily activities
- Pain that starts before your period and may last several days
- Pain that gets worse over time
- Pain during or after sex
- Bowel and bladder symptoms
This may include
- Pain when you have a bowel movement, or especially during your period
- Bloating, diarrhoea, or constipation during your period
- Blood in your stool or urine (this is less common)
- Difficulty getting pregnant
Other symptoms include:
- Persistent fatigue that doesn't improve with rest
- Mood changes, anxiety, or depression related to chronic pain
- Lower back pain during your period
Who is at Risk?
While the exact causes of endometriosis aren't fully understood, several factors may increase your risk.
They include;
Family history
You are at higher risk if your mother, sister, or other close female relatives have endometriosis.
Reproductive history
- Starting your period at a younger age (before age 11)
- Never having been pregnant or given birth
- Having shorter menstrual cycles (less than 27 days)
- Having heavier, longer periods (more than 7 days)
Other factors
- Having a low body mass index
- Being of reproductive age (typically between puberty and menopause)
Remember that having risk factors doesn't mean you will definitely develop endometriosis, and many women with endometriosis have none of these risk factors.
How Endometriosis is Diagnosed
Diagnosis of endometriosis involves the following:
Medical History
Positive history of pain as regards when it started, where you feel the pain, severity, and what makes it better or worse, how it relates to your menstrual cycle, and history of trying to get pregnant might be a pointer to endometriosis.
Physical examination
This entails a pelvic examination to check for tender areas, nodules, or signs that organs are stuck together. However, many women with endometriosis have a normal pelvic exam, so a normal pelvic exam doesn't rule out the condition.
Imaging Tests
This includes:
Transvaginal Ultrasound
A transvaginal ultrasound test uses sound waves to create images of your pelvic organs. It's particularly good at detecting ovarian cysts and some deep lesions [4].
Magnetic Resonance Imaging (MRI)
This test provides detailed images and is especially useful for detecting deep endometriosis and planning treatment.
Laparoscopy
Laparoscopy is a minimally invasive surgery where a small camera is inserted through a tiny incision in your abdomen. During this procedure, your doctor can directly see endometriosis lesions and take tissue samples to confirm the diagnosis [5]. For many years, laparoscopy was considered the only definitive way to diagnose endometriosis.
However, currently, endometriosis is diagnosed and treated based on symptoms, physical examination, and imaging results without requiring surgery first. Surgery is reserved for cases where:
- Pain is severe and not controlled by medication.
- Deep lesions are suspected.
- You are having fertility problems that might benefit from surgical treatment
- The diagnosis is uncertain
Treatment Options
There's no cure for endometriosis, but many effective treatments can help manage your symptoms and improve your quality of life. Treatment is based on:
- Your symptoms
- Age
- The extent of the disease
- Whether you want to have children in the future.
They include:
Pain Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) like Ibuprofen are often the first step for managing pain. They work best when taken at the first sign of pain, before it becomes severe. They reduce inflammation and pain.
Hormone Therapies
Hormone treatments work by reducing or stopping your menstrual periods, which decreases the activity of endometriosis tissue and relieves pain. Examples are:
Birth control pills
Combined hormonal contraceptives (pills, patches, or vaginal rings) are commonly used as a first-line treatment to reduce pain.
Progestins
These hormones can be taken as pills, injections, or through an intrauterine device and are effective at controlling pain.
Gonadotropin Releasing Hormone(GnRH) Agonists or Antagonists
These medications temporarily put you into a menopause-like state by stopping your ovaries from producing estrogen [6]. They are very effective for pain but are usually used for short periods because of side effects. Back therapy is commonly used to reduce the side effects.
Surgical Treatments
Surgery may be recommended if medications don't control your pain or if you are having fertility problems.
Conservative surgery
Laparoscopic surgery to remove or destroy endometriosis lesions while preserving your uterus and ovaries. This can reduce pain and improve fertility.
Hysterectomy
Removal of the womb (uterus), sometimes with the ovaries, may be considered if you have completed childbearing and other treatments haven't worked. Hysterectomy doesn't guarantee a cure, especially if lesions remain.
Fertility Treatments
If you are having trouble getting pregnant, your doctor may recommend:
- Surgical removal of endometriosis lesions to improve fertility.
- Assisted reproductive technologies, such as invitro fertilisation ( IVF)
The best approach depends on your age, the extent of endometriosis, and previous treatments.
What to Expect
Treatment for endometriosis is usually long–term. You may need to try different approaches or combinations of treatments to find what works best for you. Regular follow-up with your doctor is important to monitor your symptoms and adjust your treatment plan as needed.
Living With Endometriosis
Living with endometriosis can be challenging; however, strategies that can help include:
- Multidisciplinary care
Consider seeking care at an endometriosis centre or working with a team that may include a gynaecologist, physical therapists, and a mental health professional.
- Pelvic floor physical exercise
Pelvic floor exercise can help reduce pelvic pain and improve your daily function
- Mental health support
Chronic pain can affect your emotional well-being. Counselling or therapy can help you cope with the emotional impact of endometriosis.
- Connect with others
- Support groups
Connecting with other women who have endometriosis can reduce feelings of isolation and provide practical tips for managing symptoms.
- Online communities
Many organisations offer online forums and resources for women with endometriosis
Self-Management Strategies.
Keep a symptom diary
Track your pain patterns, what triggers them, and what helps. This information can guide your treatment decisions and help you communicate better with your healthcare team.
Communicate your needs
Talk openly with your employer, school, or family about how endometriosis affects you and what accommodations might help.
Lifestyle approaches
While not a substitute for medical treatment, some women find that regular exercise, stress management techniques, heat therapy, and dietary changes help manage symptoms.
Plan for the Long Term
Since endometriosis is a chronic condition, you may need to manage it for a long time. Together with your doctor, create a long-term strategy that targets:
- Pain management
- Fertility goals and timing
- Treatment side effects
- Quality of life and daily functioning
- Regular monitoring and follow–up
Conclusion
Although endometriosis is a chronic condition that can negatively impact your quality of life, the more informed you are about it, the more likely you are to receive the right care. Don't dismiss painful periods, pelvic discomfort, pain during sex, or difficulty getting pregnant. Talk to your doctor.
References
- Allaire C, Bedaiwy MA, Yong PJ. Diagnosis and management of endometriosis. CMAJ. 2023 Mar 14;195(10):E363–71. doi:10.1503/cmaj.220637 PubMed PMID: 36918177; PubMed Central PMCID: PMC10120420. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10120420/
- World Health Organization. Endometriosis [Internet]. [cited 2026 Feb 21]. Available from: https://www.who.int/news-room/fact-sheets/detail/endometriosis
- Chen LH, Lo WC, Huang HY, Wu HM. A Lifelong Impact on Endometriosis: Pathophysiology and Pharmacological Treatment. Int J Mol Sci. 2023 Apr 19;24(8):7503. doi:10.3390/ijms24087503 PubMed PMID: 37108664; PubMed Central PMCID: PMC10139092. Available from https://pmc.ncbi.nlm.nih.gov/articles/PMC10139092/
- Hsu AL, Khachikyan I, Stratton P. Invasive and non-invasive methods for the diagnosis of endometriosis. Clin Obstet Gynecol. 2010 Jun;53(2):413–9. doi:10.1097/GRF.0b013e3181db7ce8 PubMed PMID: 20436318; PubMed Central PMCID: PMC2880548. Available from https://pmc.ncbi.nlm.nih.gov/articles/PMC2880548/
- In brief: What is laparoscopy? In: InformedHealth.org [Internet] [Internet]. Institute for Quality and Efficiency in Health Care (IQWiG); 2025 [cited 2026 Feb 21]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK613276/
- Vannuccini S, Clemenza S, Rossi M, Petraglia F. Hormonal treatments for endometriosis: The endocrine background. Rev Endocr Metab Disord. 2022;23(3):333–55. doi:10.1007/s11154-021-09666-w PubMed PMID: 34405378; PubMed Central PMCID: PMC9156507. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9156507/
Disclaimer:
The information provided on this website is for general educational and informational purposes only. It is not intended to replace professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Published February 27, 2026
