Parkinson’s Disease: Signs, Causes and Treatment
Medical Writer:Judith Ewere Ojerahi RN, RM, BNSC
Medical Reviewer: Azuka Chinweokwu Ezeike, MBBS, FWACS, FMCOG, MSc (PH)
Highlights
- Parkinson’s disease is a progressive brain disorder caused by reduced dopamine that affects movement and body functions
- Its exact cause is unknown, but it involves genetic and environmental factors that damage dopamine-producing cells
- Risk factors include age, family history, male sex, and exposure to toxins
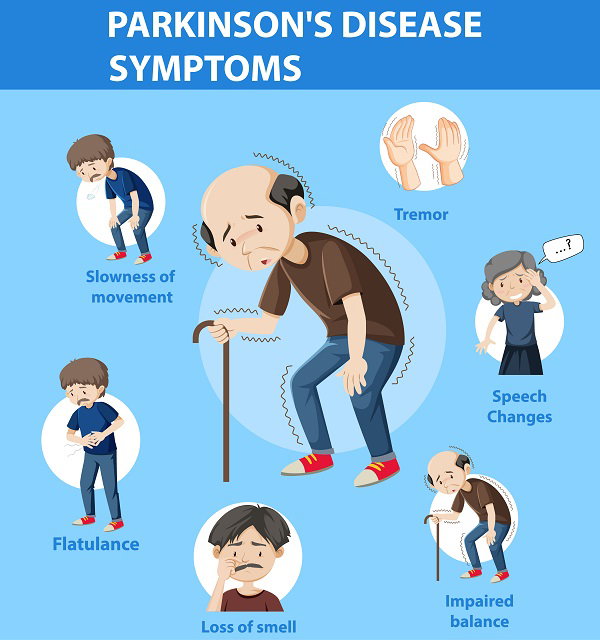
- Early signs include tremors, slow movement, muscle stiffness, and reduced facial expression
- Diagnosis is mainly based on symptoms, medical history, and neurological examination
- Treatments like levodopa, deep-brain stimulation, and supportive care help control symptoms
Introduction
Imagine waking up one day and finding out that your body moves like it has a mind of its own. For millions of people worldwide, this isn't just a thought; it's a daily reality.
Parkinson’s disease is the second most common neurodegenerative disorder after Alzheimer’s disease. It affects the brain and gradually worsens over time. It happens when certain nerve cells (neurons) in the brain become damaged or stop working properly, especially the cells that help control movement.It is usually diagnosed in people over 65. Its early signs are often so subtle that they are mistaken for normal ageing. From a slight tremor in the hand to changes in how you speak or sleep, Parkinson’s reshapes lives in different ways.
The exact cause remains unknown, but through a combination of medicine, lifestyle management, and the power of a strong support system, it is possible to maintain a high quality of life. In this article, we will discuss Parkinson’s disease, who is at risk, how to recognise the signs, and the steps you can take to manage its progress.
What is Parkinson’s Disease?
Parkinson’s disease is a long-term condition that affects the brain and mostly occurs in older adults, especially people above 65 years. It happens when some of the brain cells that help control movement gradually stop working.
Over time, this makes it harder for you to move normally. It can affect activities like walking, sleeping, speaking, and even balance. Parkinson’s can also cause other changes in the body that are not related to movement. Dopamine levels are reduced in people with Parkinson’s disease [1]. It begins gradually, affecting one side of the body and then progresses to involve the other side, and may lead to disability if not treated in time.
What Causes Parkinson’s Disease?
The primary cause of Parkinson’s disease is not fully understood, but it can be associated with:
- Ageing
- Pesticides
- Herbicides
- Certain air pollutants
- Family history
- Changes in a person's gene (mutation) [2]
Who is at Risk of Parkinson’s Disease?
You are at risk of developing Parkinson’s disease if you:
- Are 65 years and above. Parkinson’s disease can also develop earlier than 65 years
- Are a man
- Have an injury to the head
- Have a family history of Parkinson’s disease
- Have mutations or alterations in the structure of your genes
- Are constantly exposed to certain pesticides
- Have issues that affect your sleep
- Consume too much milk and dairy products [3].
Early Signs and Symptoms of Parkinson’s Disease
The signs and symptoms you may experience if you have Parkinson's disease develop slowly and may not be noticed. However, they become visible over time. These symptoms can be classified into two;
Motor symptoms
Motor symptoms are movement-related problems caused by Parkinson’s disease. It affects how your body functions physically. They include:
- Slow movement (bradykinesia),
- Slurred speech
- Difficulty in walking
- Involuntary shaking of body parts (tremors)
- Involuntary tightening of muscles, making movements difficult
- Not being able to keep good balance and posture when standing or walking
Non-motor symptoms
Non-motor symptoms are problems that affect your body but are not related to movement. They include:
- Depression
- Anxiety
- Not being able to smell properly
- Excessive sweating
- Issues with bowel movements that lead to faecal incontinence
- Feeling the need to urinate more often than usual
- Drooling
- Having pain in the joints
- A decline in brain function leading to issues with memory, thinking, learning or making decisions [4].
How Parkinson’s Disease Affects the Body
Parkinson’s disease starts gradually over time because of changes in the brain. One important change is the buildup of a protein called alpha synuclein. When this protein gathers in abnormal amounts, it can damage nerve cells in the brain.
This protein gathers in the gut (digestive system) before spreading to other parts of the body, like the brain stem, the sense of smell area, and later deeper parts of the brain. This explains why some people with Parkinson’s disease notice early symptoms like constipation, loss of smell or sleep problems years before movement problems begin.
As the protein continues to spread, it affects an important part of the brain called the substantia nigra. This area helps produce dopamine, a chemical that controls movement. When dopamine levels drop, symptoms like tremors, stiffness, and slow movement start to appear.
Research has shown that small structures inside cells, such as lysosomes, endosomes, and mitochondria (which help clean cells and produce energy) do not work properly in Parkinson’s disease.In addition, the inflammation starting from the gut may also contribute to the development of the disease.
Because of these findings, Parkinson’s disease is now understood to be more complex than just a lack of dopamine in the brain. Researchers are still studying why this harmful protein builds up in the first place [1].
How is Parkinson’s Disease Diagnosed?
There are limited laboratory tests or scans that can show that someone has Parkinson’s disease. However, your doctor will carry out some medical checkups to determine if you have Parkinson's disease. They include:
- Family history: This helps the doctor know if anyone in your family has had the disease before.
- Neurological examination: This test helps to check how well your brain, spinal cord and nerves are working. In this case, your doctor will assess how well you can control your movement, your speech, and your balance when standing or walking.
- Levodopa medication: The doctor will give you a drug called Levodopa and monitor if your symptoms improve if it is suspected that you have Parkinson’s disease.
After this examination is done, further scans can be done to identify problems in the brain. They include:
- Magnetic Resonance Imaging
- Positron Emission Tomography
- Dopamine uptake or dopamine transporter (DAT) [5].
Treatment Options for Parkinson’s Disease
There is currently no cure for Parkinson’s disease, but there are non-pharmacological options, medications and invasive treatment options that help manage the symptoms.
Non-pharmacological Options
This treatment option helps to manage the symptoms alongside the use of medications. Your healthcare provider will advise you to:
- Limit your consumption of coffee and tea at least 4 hours before sleep so that you can have adequate sleep
- Eat lots of fruits, vegetables and fibres to keep your bowels moving and avoid constipation.
- Take part in regular exercise and physical activity that significantly helps to improve your movements and ensure posture stability [6].
Medication options
Medications used to improve your movement-related symptoms include:
- Levodopa: This medication stabilises the dopamine level, thus reducing the motor movement symptoms.
- Dopamine agonist: Dopamine agonists, such as ropinirole and pramipexole, can be taken alone or together with Levodopa. These medications help to improve your movements [6].
For symptoms that do not affect your movement, like depression, anxiety, and sleep disorders, the following medication options are used to manage symptoms:
- Serotonin/norepinephrine reuptake inhibitors (SNRIs) such as fuloxetine and desvenlafaxine are used to manage depression caused by Parkinson's disease.
- Medications such as clonazepam, doxepin, eszopiclone, melatonin, and mirtazapine are used to manage sleep disturbances.
- Acetylcholinesterase inhibitors such as donepezil and galantamine help to treat a decline in brain function.
- Benzodiazepines can be used to manage anxiety. Some of these drugs include: clonazepam, diazepam, and lorazepam [6].
Invasive Treatment Options
This treatment option is considered when you have symptoms that affect how you move, control your muscles and when you show no improvement with medications.
- Deep brain stimulation: Doctors place very small wires on certain parts of the brain and connect them to a small battery device placed under the skin in the chest, which releases electrical signals to the brain and helps to control motor symptoms and muscle stiffness.
- Enteral suspension of Levodopa–carbidopa: This involves administering Levodopa-carbidopa directly into the stomach or intestine without passing through the mouth.
- Subcutaneous infusion of Apomorphine: Apomorphine is given under the skin continuously to help control the movement [6].
Living With Parkinson’s Disease
Parkinson’s disease usually begins gradually. Living with Parkinson’s disease involves managing your symptoms so they don't interfere with your usual daily activities. You can manage your symptoms by:
- Ensuring you take your medications according to your doctor's prescription, doing simple exercises like yoga, walking, and stretching, improves your balance and muscle strength.
- Consume a balanced diet rich in fruits, vegetables and fibre, as this aids in reducing gastrointestinal symptoms you may have.
- Having a good night's sleep greatly improves your well-being. Switch off the lights and avoid taking caffeine, coffee or tea that contains caffeine before sleeping.
- Keeping your space and environment safe and free from whatever can cause falls or injuries to you
- Reaching out to someone or your healthcare provider whenever you are depressed or lonely, this would benefit your mental health and wellbeing.
How to Support Someone With Parkinson’s Disease
Someone with Parkinson’s disease should be supported in ways that can improve their health. Your families and friends can support you by:
- Setting reminders to ensure you take your drugs on time and adhere to the drug prescription
- Encouraging you to participate in active games and exercises
- Providing you with digital health tools that can monitor your vital signs [7]
- Helping you make your environment free from things that can cause falls or injuries.
Factors Associated with Reduced Risk of Parkinson’s Disease
There are a few factors that can delay you developing Parkinson’s disease, especially if you are at risk of getting it. These factors include:
- Being physically active from an early age and participating regularly in physical activity can help delay the disease. Exercise can also improve balance and muscle control.
- Sleep is an underrated therapy for many disease conditions. Good sleep and rest improve brain health, which is essential in reducing the risk of Parkinson's disease.
- Having a good social network and support is known to have a positive effect on brain health
- Eating a balanced meal of fruits, vegetables, protein, carbohydrates, and vitamins serves as a protection against developing the disease
- Regular intake of vitamins D, B12, and B16
- Engaging in mentally stimulating activities. These activities protect and stimulate your brain. Some of the activities include: reading, solving puzzles, and learning a new skill [8].
When to See a Doctor
You should see a doctor when you notice that:
- One side of your body becomes stiff or tightens involuntarily,
- Your speech becomes slow, and sometimes it gets difficult to speak.,
- You have trouble sleeping,
- You are not able to perform the daily activities you normally do,
- Standing or walking becomes difficult,
- You are not able to control your bowel movements,
- Loss of smell
- Resting tremors
Conclusion
In conclusion, Parkinson’s disease is a condition that affects your brain over time, especially as you age, and it can influence both your movement and other body functions. Even though there is currently no cure, you can still live a full and meaningful life with the right management and support.
If you are living with Parkinson’s disease, you are not helpless. You can manage the symptoms and maintain a good quality of life by taking your medications as prescribed, staying physically active with regular exercise, eating a balanced and balanced diet, getting enough rest, and keeping up with medical appointments.
Having strong support from your family, friends, and healthcare providers also makes a big difference in how well you cope with the condition.
References
- Zafar S, Lui F, Yaddanapudi SS. Parkinson disease. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470193
- Bogers JS, Bloem BR, Den Heijer JM. The etiology of Parkinson's disease: new perspectives from gene-environment interactions. Journal of Parkinson’s Disease. 2023;13(8):1281–1288. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10741370/
- Prajjwal P, Flores Sanga HS, Acharya K, Tango T, John J, Rodriguez RSC, et al. Parkinson’s disease updates: addressing the pathophysiology, risk factors, genetics, diagnosis, along with the medical and surgical treatment. Annals of Medicine and Surgery (London). 2023;85:4887–4902. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10553032/
- Kouli A, Torsney KM, Kuan WL. Parkinson’s disease: etiology, neuropathology, and pathogenesis. In: Stoker TB, Greenland JC, editors. Parkinson’s disease: pathogenesis and clinical aspects [Internet]. Brisbane (AU): Codon Publications; 2018. Chapter 1. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536722/
- Khan AZ, Lavu D, Neal RD. Parkinson's disease: a scoping review of the quantitative and qualitative evidence of its diagnostic accuracy in primary care. Br J Gen Pract. 2024;74(741):e227–e232. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10962518/
- Pardo-Moreno T, García-Morales V, Suleiman-Martos S, Rivas-Domínguez A, Mohamed-Mohamed H, Ramos-Rodríguez JJ, Melguizo-Rodríguez L, González-Acedo A. Current treatments and new, tentative therapies for Parkinson's disease. Pharmaceutics. 2023;15(3):770. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10051786/
- Jones J, Ramaswamy B. Empowering people with Parkinson's: reframing self-management in Parkinson's—a critical reflection of current practice. Healthcare (Basel). 2025;13(21):2673. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC12609764/
- Beheshti I. Exploring risk and protective factors in Parkinson's disease. Cells. 2025;14(10):710. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC12110598/
- Morris HR, Spillantini MG, Sue CM, Williams-Gray CH. The pathogenesis of Parkinson's disease. Lancet. 2024 Jan 20;403(10423):293–304.Available from: https://pubmed.ncbi.nlm.nih.gov/38245249/
- Zhou ZD, Yi LX, Wang DQ, Lim TM, Tan EK. Role of dopamine in the pathophysiology of Parkinson's disease. Transl Neurodegener. 2023 Sep 18;12(1):44. Available from:https://pmc.ncbi.nlm.nih.gov/articles/PMC10506345/
Disclaimer:
The information provided on this website is for general educational and informational purposes only. It is not intended to replace professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Published April 20, 2026

